Educational Appendix
Antibody Drug Nomenclature
The nomenclature of monoclonal antibodies is a naming scheme for assigning generic, or nonproprietary, names to monoclonal antibodies. This naming scheme is used for both the World Health Organization's International Nonproprietary Names (INN) and the United States Adopted Names (USAN) for pharmaceuticals. In general, word stems are used to identify classes of drugs, in most cases placed at the end of the word. All monoclonal antibody names end with the stem -mab. Unlike most other pharmaceuticals, monoclonal antibody nomenclature uses different preceding word parts (morphemes) depending on structure and function. These are officially called substems.
List of stems for monoclonal antibody nomenclature
| Prefix | Target substem | Source substem | Stem | |||
|---|---|---|---|---|---|---|
| old | new | meaning | meaning | |||
| variable | -anibi- | — | angiogenesis (inhibitor) | -a- | rat | -mab -pab |
| -ba(c)- | -b(a)- | bacterium | -e- | hamster | ||
| -ci(r)- | -c(i)- | circulatory system | -i- | primate | ||
| -fung- | -f(u)- | fungus | -o- | mouse | ||
| -gr(o)- | -gr(o)- | growth factor | -u- | human | ||
| -ki(n)- | -k(i)- | interleukin | -xi- | chimeric (human/foreign) | ||
| -les- | — | inflammatory lesions | -zu- | humanized | ||
| -li(m)- | -l(i)- | immune system | -vet- | veterinary | ||
| -mul- | — | musculoskeletal system | -xizu-* | chimeric/humanized hybrid | ||
| -ne(u)(r) | -n(e)-* | nervous system | -axo- |
rat/mouse hybrid (see trifunctional antibody) |
||
| -os- | -s(o)- | bone | ||||
| -toxa- | -tox(a)- | toxin | ||||
| -co(l)- | -t(u)- | colonic tumor | ||||
| -go(t)- | testicular tumor | |||||
| -ma(r)- | mammary tumor | |||||
| -me(l)- | melanoma | |||||
| -pr(o)- | prostate tumor | |||||
| -tu(m)- | miscellaneous tumor | |||||
| -vi(r)- -vi(r)- | -v(i)- | virus | ||||
Components
Stem
The stem -mab is used for monoclonal antibodies as well as for their fragments, as long as at least one variable domain (the domain that contains the target binding structure) is included.[1] This is the case for antigen binding fragments and single-chain variable fragments, among other artificial proteins. Other antibody parts (such as Fc regions) and antibody mimetics use different naming schemes.
Substem for origin/source
The substem preceding the stem denotes the animal from which the antibody is obtained.[1] The first monoclonal antibodies were produced in mice (substem -o-, yielding the ending -omab; usually Mus musculus, the house mouse) or other non-human organisms. Neither INN nor USAN has ever been requested for antibodies from rats (theoretically -a-), hamsters (-e-) and primates (-i-).
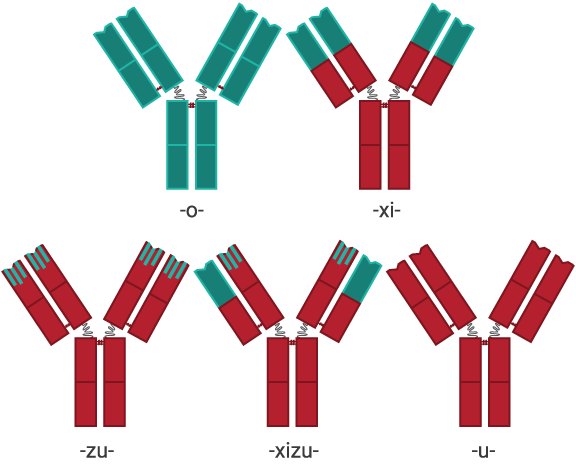
Non-human antibodies are recognized as foreign by the human immune system and may be rapidly cleared from the body, provoke an allergic reaction, or both.[2][3] To avoid this, parts of the antibody can be replaced with human amino acid sequences, or fully human antibodies can be engineered. If the constant region is replaced with the human form, the antibody is termed chimeric and the substem used is -xi-. Part of the variable regions may also be substituted, in which case it is called humanized and -zu- is used; typically, everything is replaced except the complementarity determining regions (CDRs), the three loops of amino acid sequences at the outside of each variable region that bind to the target structure. Partly chimeric and partly humanized antibodies use -xizu-. These three substems do not indicate the foreign species used for production. Thus, the human/mouse chimeric antibody basiliximab ends in -ximab just as the human/macaque antibody gomiliximab. Pure human antibodies use -u-.[4]
Rat/mouse hybrid antibodies can be engineered with binding sites for two different antigens. These drugs, termed trifunctional antibodies, have the substem-axo-.[5]
Source substems: mouse (top left), chimeric (top right), humanized (bottom left), chimeric/humanized (bottom middle), and human (bottom right) monoclonal antibodies. Human parts are shown in red, non-human parts in blue.
Substem for target
The substem preceding the source of the antibody refers to the medicine's target. Examples of targets are tumors, organ systems like the circulatory system, or infectious agents like bacteria or viruses. The term target does not imply what sort of action the antibody exerts. Therapeutic, prophylactic and diagnostic agents are not distinguished by this nomenclature.
In the naming scheme as originally developed, these substems mostly consist of a consonant, a vowel, then another consonant. The final letter may be dropped if the resulting name would be difficult to pronounce otherwise. Examples include -ci(r)- for the circulatory system, -li(m)- for the immune system (lim stands for lymphocyte) and -ne(r)- for the nervous system. The final letter is usually omitted if the following source substem begins with a consonant (such as -zu- or -xi-), but not all target substems are used in their shortened form. -mul-, for example, is never reduced to -mu- because no chimeric or humanized antibodies targeting the musculoskeletal system ever received an INN. Combination of target and source substems results in endings like -limumab (immune system, human) or -ciximab (circulatory system, chimeric, consonant r dropped).[1]
New and shorter target substems were adopted in 2009. They mostly consist of a consonant, plus a vowel which is omitted if the source substem begins with a vowel. For example, human antibodies targeting the immune system receive names ending in -lumab instead of the old -limumab. Some endings like -ciximab remain unchanged.[4] The old system employed seven different substems for tumor targets, depending on the type of tumor. Because many antibodies are investigated for several tumor types, the new convention only has -t(u)-.[1]
Prefix
The prefix carries no special meaning. It should be unique for each medicine and contribute to a well sounding name.[4] This means that antibodies with the same source and target substems are only distinguished by their prefix. Even antibodies targeting exactly the same structure are differently prefixed, such as the adalimumab and golimumab, both of which are TNF inhibitors but differ in their chemical structure.[6]
Additional words
A second word following the name of the antibody indicates that another substance is attached,[4] which is done for several reasons:
- An antibody can be PEGylated (attached to molecules of polyethylene glycol) to slow down its degradation by enzymes and to decrease its immunogenicity;[7] this is shown by the word pegol as in alacizumab pegol.[8]
- A cytotoxic agent can be linked to an anti-tumor antibody for drug targeting purposes. The word vedotin, for example, stands for monomethyl auristatin E which is toxic by itself but predominantly affects cancer cells if used in conjugates like glembatumumab vedotin.[9]
- A chelator for binding a radioisotope can be attached. Pendetide, a derivative of pentetic acid, is used for example in capromab pendetide to chelate indium-111.[10] If the drug contains a radioisotope, the name of the isotope precedes the name of the antibody.[4] Consequently, indium (111In) capromab pendetide is the name for the above example including indium-111.[10]
History
The World Health Organization (WHO) introduced the system of International Nonproprietary Names in 1950, with the first INN list being published three years later. The stem -mab for monoclonal antibodies was proposed around 1990, and the current system with target and source substems was developed between 1991 and 1993. Due to the collaboration between the WHO and the United States Adopted Names Council, antibody USANs have the same structure and are largely identical to INNs. Until 2009, more than 170 monoclonal antibodies received names following this nomenclature.[11]
In October 2008, the WHO convoked a working group to revise the nomenclature of monoclonal antibodies, to meet challenges discussed in April the same year. This led to the adoption of the new target substems in November 2009. In spring 2010, the first new antibody names were adopted.
Examples
New convention
- Olaratumab is an antineoplastic. Its name is composed of the components olara-t-u-mab. This shows that the drug is a human monoclonal antibody acting against tumors.
- The name of benralizumab, a drug designed for the treatment of asthma, has the components benra-li-zu-mab, marking it as a humanized antibody acting on the immune system.
Old convention
- Adalimumab is a drug targeting TNF alpha. Its name can be broken down into ada-lim-u-mab. Therefore, the drug is a human monoclonal antibody targeting the immune system. If adalimumab had been named after 2009, it would have been adalumab.[6]
- Abciximab is a commonly used medication to prevent platelets from clumping together. Broken down into ab-ci-xi-mab, its name shows the drug to be a chimeric monoclonal antibody used on the cardiovascular system. This and the following two names would look the same if the new convention were applied.[12]
- The name of the breast cancer medication trastuzumab can be analyzed as tras-tu-zu-mab. Therefore, the drug is a humanized monoclonal antibody used against a tumor.[13]
- Alacizumab pegol is a PEGylated humanized antibody targeting the circulatory system.[8]
- Technetium (99mTc) pintumomab and technetium (99mTc) nofetumomab merpentan are radiolabeled antibodies, merpentan being a chelator that links the antibody nofetumomab to the radioisotope technetium-99m.[14]
- Rozrolimupab is a polyclonal antibody. Broken down into rozro-lim-u-pab, its name shows the drug to be a human polyclonal antibody acting on the immune system. The suffix -pab shows it is a polyclonal antibody.
Deviations
- The monoclonal antibody muromonab-CD3, approved for clinical use in 1986, was named before these conventions took effect, and consequently its name does not follow them. Instead, it is a contraction from "murine monoclonal antibody targeting CD3".
References
- AMA (USAN) Monoclonal antibodies". United States Adopted Names. 2007-08-07.
- Stern, M.; Herrmann, R. (2005). "Overview of monoclonal antibodies in cancer therapy: present and promise". Critical Reviews in Oncology/Hematology 54(1): 11-29.
- Tabrizi M. et al. (2006) Elimination mechanisms of therapeutic monoclonal antibodies. Drug Discovery Today 11(1-2): 81-88.
- General policies for monoclonal antibodies. World Health Organization.
- Lordick F et al. (2008) The evolving role of catumaxomab in gastric cancer. Expert Opinion on Biological Therapy 8(9): 1407-15.
- Miyasaka, N (2009) Adalimumab for the treatment of rheumatoid arthritis. Expert Review of Clinical Immunology 5(1): 19-22.
- Veronese F and Pasut G (2005) PEGylation, successful approach to drug delivery. Drug Discovery Today 10(21): 1451-1458.
- "International Nonproprietary Names for Pharmaceutical Substances (INN)" (PDF). WHO Drug Information (World Health Organization) 22(3): 221. 2008.
- "Drug Dictionary: Glembatumumab vedotin". National Cancer Institute.
- "ATC/DDD Classification (final)". WHO Drug Information (World Health Organization) 15(2). 2001.
- "International Nonproprietary Names". Drugs.com.
- "Abciximab". Drugs.com.
- "Trastuzumab". Drugs.com.
- "International Nonproprietary Names (INN) for Pharmaceutical Substances: Names for radicals & groups comprehensive list" (PDF). World Health Organization. 2002. p. 22.
